Degenerative Arthritis
Degenerative arthritis affects millions of people across the globe. You may have heard it called osteoarthritis, degenerative joint disease or wear and tear arthritis. No matter which name you give it, degenerative arthritis is something to keep on your radar.
What Is Degenerative Arthritis?
Degenerative arthritis is the most common type of arthritis. By the numbers, degenerative arthritis affects nearly all people in some way by age 80 since it’s primarily a disease of aging. Regular and overuse of specific joints cause the cartilage to break down.
Cartilage is a slippery tissue that enables nearly frictionless joint motion. As the cartilage wears away over time (or with overuse), more friction is the result, and the rubbing forms a rough, pitted surface on previously smooth cartilage.
If the cartilage deteriorates completely, your bones will rub against each other. The joint is no longer able to move without friction and results in significant arthritic pain.
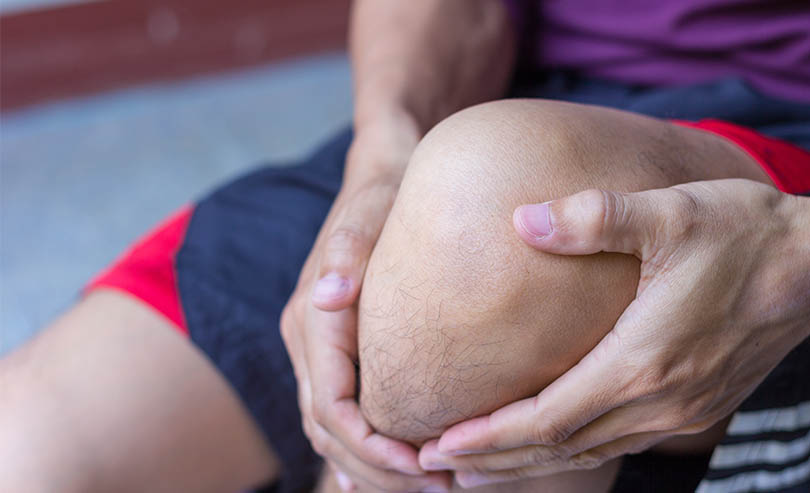
Degenerative arthritis commonly affects the hands, knees, hips, and spine but can damage any joint.
Symptoms of Degenerative Arthritis
Several symptoms may be the result of degenerative arthritis. Symptoms can be managed, but the joint damage can’t be reversed, so if you’re noticing some minor symptoms now – it’s important to have a medical professional assess you right away.
Symptoms develop slowly, usually starting in one or two joints. Arthritis symptoms gradually worsen as time goes on, especially if the patient is not seeking treatment. Symptoms are generally worse in the morning and after periods of inactivity.
Common symptoms may include:
- Pain that may come and go
- Soft tissue inflammation around the joint, which can result in swelling; swelling makes the joint feel tender and sore.
- The affected joints may have periods of stiffness and immobility
- As this type of arthritis progresses, new growths of bone, called bone spurs, can form around the joint. They feel like hard lumps and make the joints more enlarged and cause aggravating pain and loss of mobility
- Joints may hurt during and after movement
- Joints may feel tender when you apply light pressure on or around it
- Loss of flexibility which means your full range of motion may no longer be reached
- There may be a grating sensation when you use the joint
- You may hear a popping/cracking sound when you use the joint
- Muscle weakness around the joint is common, especially for arthritis in the knee
- As degenerative arthritis progresses, joints may start to become crooked or deformed
A gluten-free diet for arthritis can be beneficial because it can help reduce inflammation. Here are the common gluten-free foods to consume.
Risk Factors
- Obesity – Extra weight adds stress to your weight-bearing joints. Fat tissue also produces proteins that cause inflammation in and around your joints. Try switching to a healthier lifestyle by incorporating physician-recommended exercise and diet.
- Demanding sports – Repetitive stress to a joint may cause the joint to develop degenerative arthritis. This strain is hard to predict, so if you’re playing high-intensity sports that strain your joints, get a medical opinion or assessment regarding your risk of joint damage.
- Older age – Since the likelihood of acquiring degenerative arthritis increases with age, those who are older are more prone
to develop it. - Sex – Women more likely to develop degenerative arthritis, but the reason why is not clear. However, men are more prone to develop degenerative arthritis due to injury.
- Joint injuries – Injuries to the joint, even one that happened ages ago and seemed to have healed, can increase your risk of degenerative arthritis. If you’ve experienced a serious joint injury, have it reassessed to see if you should be concerned about this type of arthritis in the future.
- Heredity – Some people can inherit genes that make them more prone to degenerative arthritis. This risk factor comes down to the genetic cards you’re dealt with. If degenerative arthritis runs in your family, stay aware of any joint issues you start to experience and let your doctor know.
Treatment for Degenerative Arthritis
Early treatment is vital because it limits the progression of degenerative arthritis. Treatment usually includes a combination of physical therapy exercises and medical therapy.
Physical Therapy
Physical therapy strengthens muscles around the affected joint. This type of therapy also helps you learn to cope with any limitations and find ways to avoid putting additional stress on the affected joint. Pain management and stress management classes can also help those diagnosed with arthritis.
Medication
Your doctor may advise that you take medications, including topical creams, acetaminophen, NSAIDs (like Advil), glucosamine, and cortisone injections, to name a few options. Sometimes injections are used to reduce pain and maintain mobility/flexibility of the joints.
Your doctor will determine the medication and administration of injections. Prescriptions for these depend on current medications you’re taking, pain levels, and other factors.
Surgery
Surgery may be an option in later stages. Surgery is used to relieve pain and attempts to prevent progressive weakness and deformity. There are three common types available:
- Fusion – An operation that makes the bones on each side of a joint grow together. This method is helpful for stiff/painful joints or joints that are awkwardly crooked or unstable.
- Joint reconstruction – Artificial joints have been developed for small joints in the fingers and thumb. Reconstruction is an alternative to fusion. In some cases, reconstruction can restore motion to a joint which has been previously fused.
- Osteotomy – Cutting bones in order to realign them in a way that promotes pain-free movement. This option can reduce wear and tear on the cartilage that has been damaged.
The Bottom Line...
As we age, our bodies are bound to change, and from years of joint use, we may be heading toward degenerative arthritis in the future.
Staying active, maintaining a healthy weight, and some treatments may slow the development of degenerative arthritis while at the same time help improve joint pain and function.
Take care of your joints, and if you have any concerns about this type of arthritis, see your doctor for some tips on prevention.